
GPT-5
Your morning coffee may do more than just wake you up—it might also weaken donated blood. A recent large study reveals that caffeine reduces the quality of red blood cells, which can make transfusions less effective, particularly for patients who rely on them the most.
Worldwide, around one billion people—about 12.6% of the global population—drink coffee. People around the world consume over 2.25 billion cups of coffee each day, giving a caffeine boost to roughly 12.6% of the global population.
While caffeine has generally been shown to have health benefits, a new study led by the University of Colorado Anschutz Medical Campus reveals that caffeine may lower the quality of donated blood and reduce its effectiveness during transfusions.
“We’ve long known about caffeine’s effects on the brain and central nervous system, but this is the first large-scale study to show its impact on red blood cell biology,” said Angelo D’Alessandro, PhD, professor of biochemistry at the University of Colorado School of Medicine and the study’s corresponding author. “These results suggest that something as common as your morning coffee could significantly affect the quality of stored blood and its performance when transfused into patients.”
Analyzing Blood Composition and the Impact of Caffeine on Red Blood Cells
Blood consists of plasma—a straw-colored fluid—and formed elements, which include red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes). Plasma, containing water, proteins, sugars, and other components, accounts for about 55% of blood volume, while the formed elements make up the remaining 45%, suspended within the plasma.
As part of the large US blood bank study REDS RBC-Omics, researchers analyzed red blood cells from 13,091 blood donors. They measured caffeine levels in stored blood and examined its effects on red blood cell metabolism, hemolysis (cell rupture), and transfusion results. Researchers recalled 643 donors with either very high or very low red blood cell fragility to donate blood again, enabling them to study the samples over different storage periods: 10, 23, and 42 days.
Eight healthy volunteers each drank a cup of coffee, and their blood was tested before and after to observe caffeine’s immediate effects on red blood cells. In the lab, researchers studied how caffeine affected important RBC pathways, focusing on ADORA2b signaling—a receptor that helps RBCs respond to stress and low oxygen levels—and G6PD enzyme activity, which protects RBCs from oxidative damage. To confirm these mechanisms, mice genetically engineered to lack ADORA2b were also studied, examining how caffeine exposure influenced their red blood cells’ recovery after transfusion.
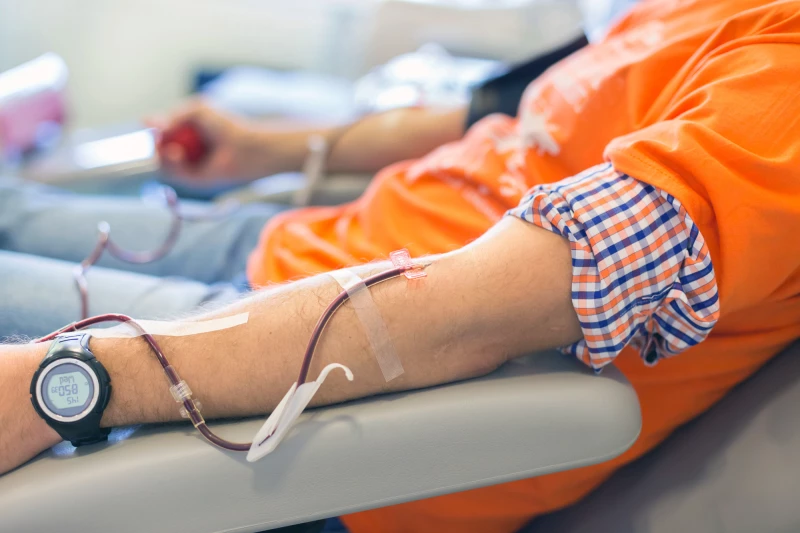
Depositphotos
Caffeine’s Impact on Red Blood Cell Stability and Oxygen Delivery
Many blood donors had detectable levels of caffeine in their red blood cells, with levels remaining consistent across multiple donations—particularly among regular coffee drinkers. Researchers found that higher caffeine levels correlated with reduced amounts of two key molecules: adenosine triphosphate (ATP) and 2,3-bisphosphoglycerate (2,3-BPG). Since red blood cells lack a nucleus and mitochondria—the usual machinery for generating energy—they depend on a small set of chemical “fuel molecules” to survive and function. ATP and 2,3-BPG are among the most essential for this purpose.
The study also showed that caffeine made red blood cells more fragile and more likely to rupture under stress, while increasing signs of oxidative damage. After transfusion, blood from donors with higher caffeine levels resulted in smaller increases in patients’ hemoglobin. In short, caffeine appeared to deplete the cells’ energy reserves and weaken their ability to deliver oxygen effectively throughout the body.
Donors with common genetic variants in the ADORA2b gene experienced even poorer outcomes when caffeine was present, making their stored red blood cells particularly vulnerable. In mice lacking ADORA2b, red blood cells were already fragile, and adding caffeine during storage worsened the issue. This revealed a “double hit” effect: caffeine both blocked ADORA2b signaling and directly inhibited the G6PD enzyme, which weakened the cells’ antioxidant defenses.
“Our findings have major real-world implications,” said D’Alessandro. “Caffeine consumption—something up to 75% of Americans regularly do—appears to be a modifiable lifestyle factor that can impact red blood cell storage quality and transfusion effectiveness. Since caffeine has a short half-life in the body, temporary dietary changes around the time of blood donation could reduce its harmful effects. This idea already aligns with blood donation guidelines in parts of Europe, where donors are advised to limit caffeine intake before giving blood.”
Study Limitations and Potential for Personalized Blood Donation Strategies
The study had some limitations. Only eight participants drank coffee for the metabolic testing, and all had prior caffeine exposure—none were caffeine-naïve. The donor blood samples used were about a decade old; although storage techniques have remained largely the same, donor demographics or habits might have changed over time. Additionally, red blood cell physiology in mice differs from that in humans. While the effect on transfusion outcomes was relatively modest, the potential risk for individual patients appears low but could still be significant when considered across a larger population.
The study points to intriguing real-world implications, especially regarding blood donations for transfusions. A more personalized approach—considering donor lifestyle factors like caffeine intake and genetic traits such as ADORA2b variants—could help better match donors to recipients and improve transfusion results. For vulnerable patients, such as newborns or those in critical condition, receiving blood from low-caffeine donors might lead to better outcomes.
Read the original article on: New Atlas
Read more: Anxiety Could Be Naturally Embedded in The Brain During Pregnancy
