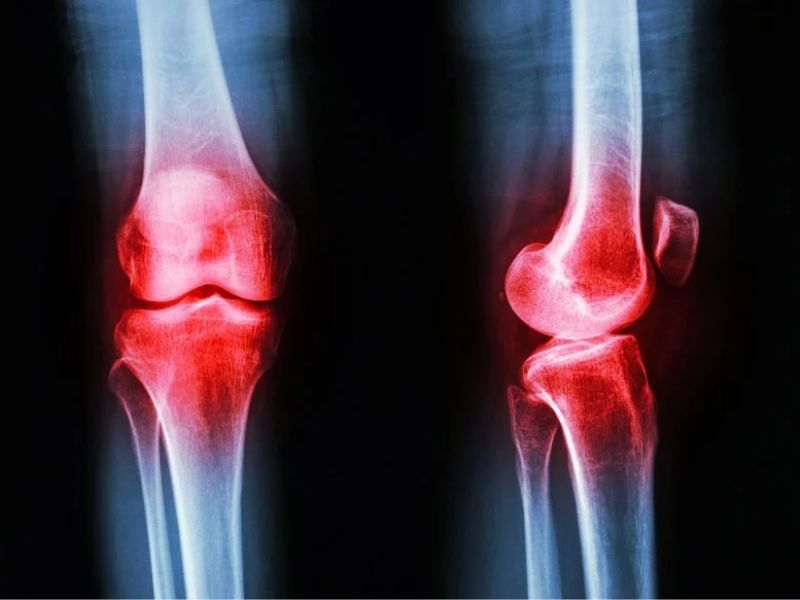
A comprehensive review of clinical research is raising questions about one of the most frequently recommended treatments for osteoarthritis.
For the millions affected by the condition, advice to exercise is almost automatic in routine care. However, a new analysis indicates that its impact on reducing joint pain and improving daily function may be more modest—and more short-term—than many patients anticipate.
Writing in the open-access journal RMD Open, researchers conclude that exercise therapy likely offers only small, temporary improvements in osteoarthritis symptoms and, in some comparisons, may be no more effective than no treatment at all. Their findings draw on both an umbrella systematic review and a pooled analysis of existing data.
The researchers say their findings call into question the routine promotion of exercise as a universal first-line treatment for all people with osteoarthritis. They suggest the field may need to reconsider which research priorities take center stage, including which therapies warrant more rigorous head-to-head comparisons and extended follow-up periods.
Exercise is commonly recommended early in the course of various types of osteoarthritis. Still, the authors note that a growing number of studies have begun to question the true strength and durability of its benefits.
While numerous systematic reviews have examined exercise for osteoarthritis, the team emphasizes that no single, wide-ranging analysis has evaluated it against a full array of alternatives—such as placebo, standard care, no intervention, medications, other non-drug approaches, and surgery.
Review Scope and Methodology
To fill this gap, the researchers searched major medical databases for relevant systematic reviews and randomized controlled trials published through November 2025. Their umbrella review incorporated five systematic reviews totaling 8,631 participants, along with 28 randomized trials that included 4,360 participants. Most of these studies centered on knee or hip osteoarthritis (23 trials), while a smaller number addressed hand (3) and ankle (2) osteoarthritis.
After combining and analyzing the data, the researchers found that exercise produced modest, short-term reductions in knee osteoarthritis pain compared with placebo or no treatment. However, the overall certainty of the evidence was judged to be very low. In larger trials and those with longer follow-up, the observed benefits were even more limited.
Moderate-certainty evidence suggested that exercise had minimal to no impact on hip osteoarthritis and only modest benefits for hand osteoarthritis.
Results with differing levels of certainty indicated that exercise yielded outcomes comparable to patient education, manual therapy, pain medications, corticosteroid or hyaluronic acid injections, and arthroscopic knee surgery.
In some subgroups examined within individual trials, exercise proved less effective over the long term than knee osteotomy and joint replacement procedures.
Study Limitations and Interpretation
The researchers admit they selectively prioritized certain reviews for inclusion, which left out some relevant studies. However, additional analyses of effect sizes from the excluded reviews yielded similar results.
They also point out that few studies directly compared exercise with other treatments. Participant characteristics varied widely, and some trials allowed additional therapies alongside exercise, which could have influenced outcomes.
Despite these limitations, they conclude: Overall, the evidence on exercise for osteoarthritis is largely inconclusive, showing minimal—or at best, short-term—effects on pain and function across different types of osteoarthritis compared with placebo or no treatment. Benefits appear smaller in larger, longer-term trials.
“These findings challenge the routine promotion of exercise as the sole first-line therapy for improving pain and physical function in all osteoarthritis patients.”
The researchers emphasize that osteoarthritis management extends beyond joint symptoms. Exercise can still benefit heart health, mood, sleep, balance, and independence, and many patients prefer it over medications or procedures. They recommend a more individualized approach rather than abandoning exercise entirely.
“They recommend that clinicians and patients make treatment decisions together, considering not only the modest effects of exercise on pain and function but also its secondary health benefits, safety, affordability, stage of care, and other available treatment options.”
Read the original article on: SciTechDaily
Read more: Japanese Scientists Developed Tech to Record and View Dreams