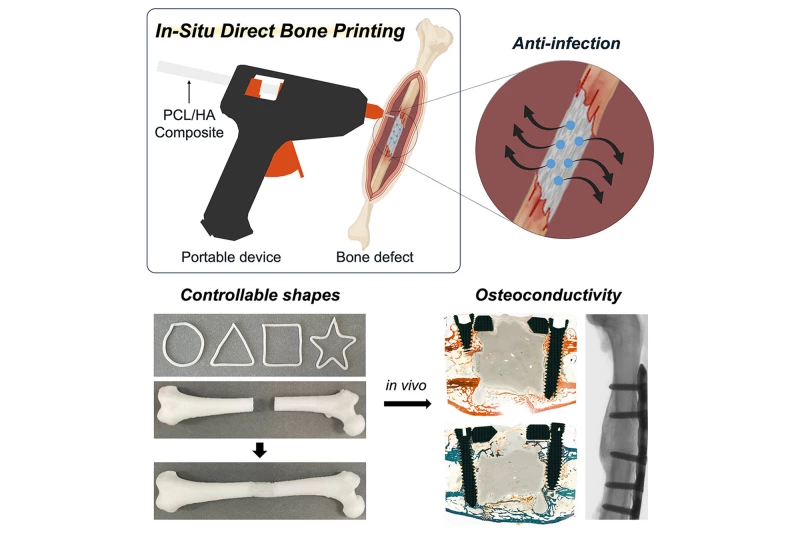
Chinese researchers have developed 3D-printed bioglass that matches bone strength, supports cell survival for weeks, and could transform customized dental implants.
Glass is rarely thought of as a replacement for human bone, but Chinese scientists suggest it may be possible. They have created a bioactive, 3D-printable glass that replicates bone strength. Tests showed it supports cell growth longer than conventional glass and performs nearly as well as materials currently used in dental implants.
How Glass Mirrors Bone
Glass and bone have a key trait in common: they withstand compression more effectively than tension. This shared property has inspired new and ambitious research.
Silica, the primary component of glass, becomes easily shapeable when molten, allowing implants to be formed to precisely match damaged skeletal areas.
However, a major challenge remained: conventional glass 3D-printing methods rely on toxic plastic additives and temperatures exceeding 2,000°F, making them impractical for medical applications where safety and affordability are critical.
The team led by Jianru Xiao, Tao Chen, and Huanan Wang pursued a safer approach by blending silica particles with calcium and phosphate ions—both known to encourage bone cell growth.
Printing Without Toxic Additives
The resulting mixture formed a printable gel that solidified at 690°C, eliminating the need for toxic additives used in traditional methods.
To evaluate its performance, the researchers tested three materials: the new bioglass, standard silica glass, and a commercial dental bone substitute, using them to repair skull defects in rabbits.
Although the commercial material triggered quicker early growth, the bioglass proved more durable. After eight weeks, many bone cells remained firmly bonded to the bioglass framework, while ordinary glass showed little to no cell attachment.
The breakthrough extended beyond medicine to the manufacturing process itself. The researchers emphasized the technical advantages of their approach.
Challenges of Conventional 3D Printing
Traditional ceramic and glass 3D printing relies on organic binders and extremely high temperatures, driving up costs, reducing bioactivity, and posing potential toxic hazards.
In contrast, the team used inorganic colloidal gels composed of silica nanospheres that bind through electrostatic attraction. This method enabled the creation of strong, additive-free structures, completed using relatively low heat via low-temperature sintering.
The results were notable: the material achieved a compression modulus of about 2.3 MPa—enough to support bone. It also retained self-healing properties, improving print stability and precision.
Promoting Real Bone Growth
After sintering at 600°C, the printed structures remained stable, bioactive, and capable of promoting new bone growth in real-world tests.
The researchers claim their approach opens the door to personalized, cost-effective, and high-performance implants.
“The ‘green’ inorganic 3D printing method allowed affordable production of bioglass bone substitutes while maintaining bioactivity, enhancing bone formation and integration in vivo,” the authors explained.
They also noted that the technique could be applied beyond medicine, including in energy and machinery industries.
The complete study appeared in the journal ACS Nano.
Read the original article on:Clickpetroleoegas
Read more:Astronauts Splash down on Earth after a Space Station Medical Evacuation