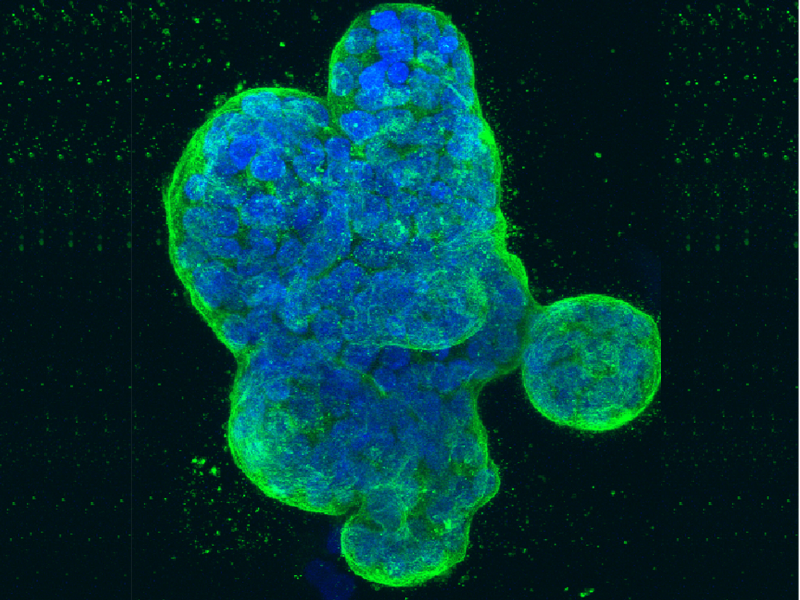
Studies suggest that melittin, a substance found in bee venom, could potentially kill aggressive breast cancer cells.
Recent studies indicate that bee venom could play a role in combating breast cancer.
Researchers are particularly interested in melittin, the primary component of Apis mellifera venom, which has demonstrated encouraging effects against aggressive forms of breast cancer, notably triple-negative and HER2-positive types.
How Does Melittin Exert its Effects?
Researchers at the Harry Perkins Institute of Medical Research in Australia report that melittin can eliminate up to 100% of tumor cells within 60 minutes while causing minimal harm to healthy cells.
In this way, the compound acts by inhibiting receptors involved in tumor growth, like EGFR and HER2, thereby halting the proliferation of cancer cells.
Lab-made versions of the substance produced nearly identical effects, further supporting its potential as a therapeutic agent.
New Progress
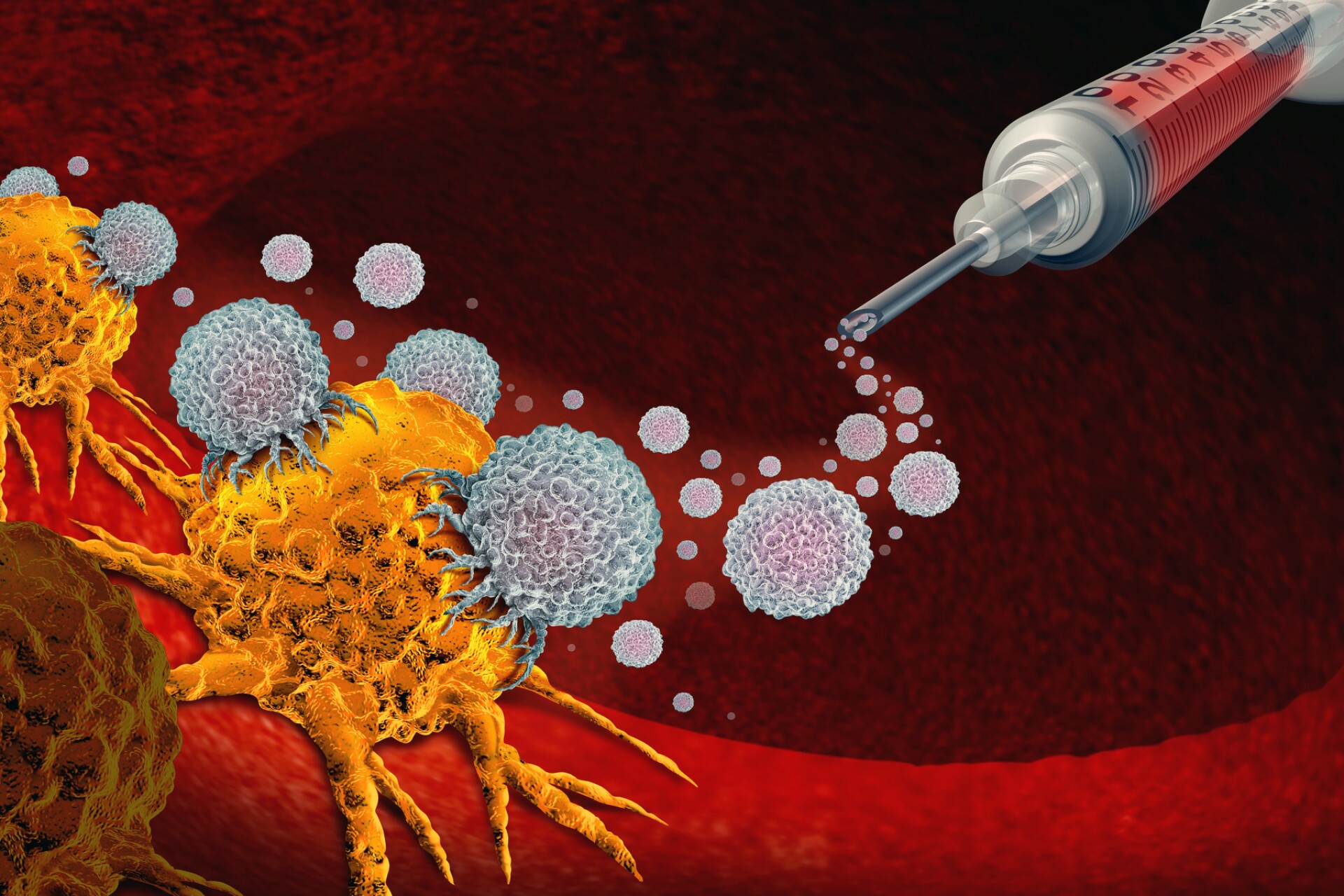
In 2025, scientists at the same institute unveiled an injectable version of melittin. Newsweek reported that in preclinical trials, this approach destroyed tumor cells within six hours and sustained its effects for a week.
Moreover, when applied directly to tumors, it selectively attacked cancer cells while leaving healthy tissue intact.
Nevertheless, experts caution that extensive research over several years is still required before the therapy can be tested in humans.
Expected Gains and Hazards
Laboratory studies have suggested several potential benefits, including:
- Quick elimination of cancer cells
- Minimal harm to healthy cells
- Possible enhancement of chemotherapy effectiveness
- Lower risk of cancer spreading
However, these findings remain preclinical.
Accordingly, UCLA Health cautions that melittin can be highly toxic and that apitherapy—the use of bee venom as an alternative treatment—lacks scientific support and may trigger serious reactions, including anaphylactic shock.
What are The Potential Developments Ahead?
Research on melittin as a potential breast cancer treatment is ongoing, with the current focus on finding safe and effective ways to administer it.
However, experts stress that, for now, bee venom should not be used as a substitute for standard therapies.
Read the original article on: Versatilis
Read more: Scientists Create a Synthetic Leaf that Turns Pollution into Energy