A recent study indicates that a common respiratory bacterium could have an unexpected connection to Alzheimer’s disease.
Researchers at Cedars-Sinai are investigating an unexpected source for Alzheimer’s disease clues: the eye. In a study published in Nature Communications, they show that Chlamydia pneumoniae—a bacterium best known for causing pneumonia and sinus infections—can persist in the body for years and may contribute to changes seen in Alzheimer’s disease.
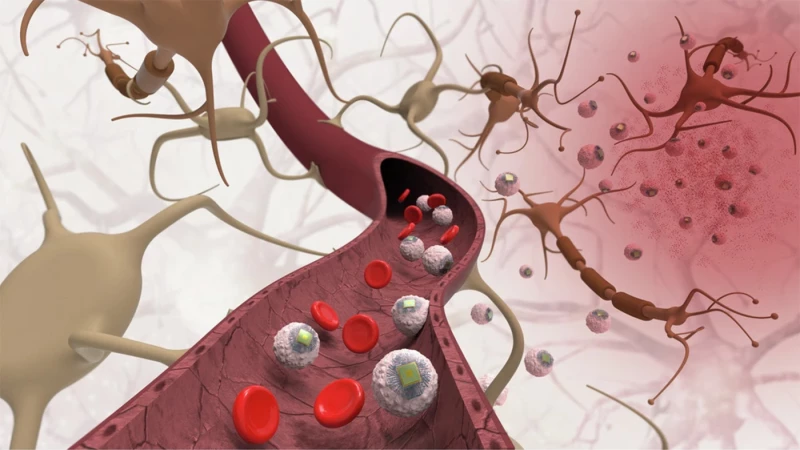
The findings suggest that a long-term infection could contribute to the inflammation that harms nerve cells and point to potential new interventions, ranging from strategies that limit inflammation to earlier antibiotic treatments.
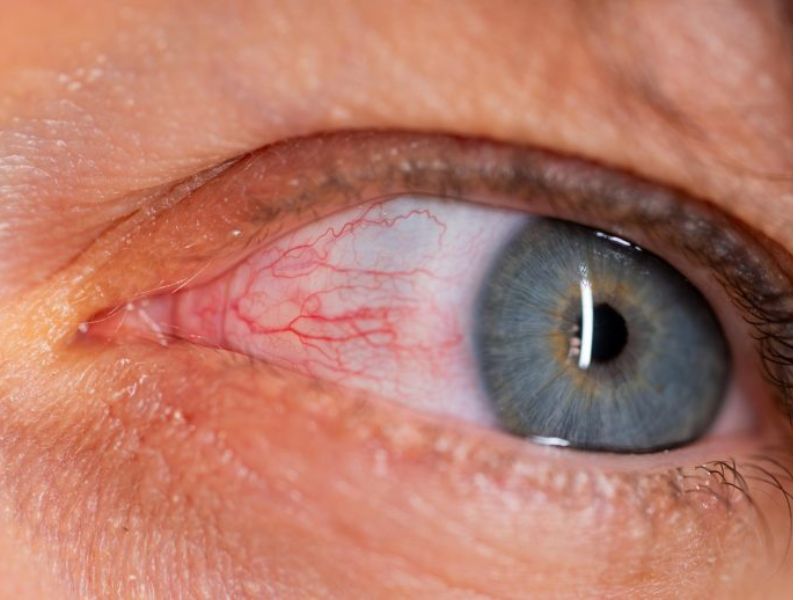
The study revealed that the bacterium can appear in the retina, the thin layer of neural tissue at the back of the eye responsible for processing visual signals. Since the retina forms part of the central nervous system and researchers can examine it without surgery, it offers a unique opportunity to observe brain-related processes in real time. The researchers found that when Chlamydia pneumoniae reaches the retina, it is associated with immune responses tied to inflammation, nerve cell damage, and cognitive decline.
Connecting Infection, Inflammation, and Nerve Cell Damage
“Observing Chlamydia pneumoniae consistently across human tissues, cell cultures, and animal models allowed us to uncover a previously unrecognized connection between bacterial infection, inflammation, and neurodegeneration,” said Maya Koronyo-Hamaoui, PhD, professor of Neurosurgery, Neurology, and Biomedical Sciences at Cedars-Sinai Health Sciences University and the study’s senior author. “The eye serves as a proxy for the brain, and our findings show that bacterial infection in the retina and ongoing inflammation can mirror brain pathology and indicate disease progression, supporting the use of retinal imaging as a noninvasive tool to identify individuals at risk for Alzheimer’s.”
To explore this, the team used advanced imaging along with genetic and protein analyses to study retinal tissue from 104 participants, including those with normal cognition, mild cognitive impairment, and Alzheimer’s disease.
They found significantly higher levels of Chlamydia pneumoniae in the retinas and brains of participants with Alzheimer’s compared with those with normal cognition, and greater bacterial presence correlated with more severe brain changes and cognitive decline.
Genetics also seemed to play a role, with elevated bacterial levels occurring more frequently in individuals carrying the APOE4 gene variant, a recognized risk factor for Alzheimer’s disease.
Results from Laboratory and Animal Studies
Investigators also studied human neurons in the lab and in laboratory mice with Alzheimer’s disease. In both, infection with Chlamydia pneumoniae increased inflammation, nerve cell death and cognitive decline, showing the bacterium can accelerate disease processes. The infection also triggered production of amyloid-beta, the protein that accumulates in the brains of people with Alzheimer’s.
The findings were driven by co-first authors Bhakta Gaire, PhD, and Yosef Koronyo, MSc.
“This discovery raises the possibility of targeting the infection-inflammation axis to treat Alzheimer’s,” said Timothy Crother, PhD, co-corresponding author of the study and research professor at Cedars-Sinai Guerin Children’s and the Department of Biomedical Sciences at Cedars‑Sinai.
Results from Laboratory and Animal Studies
The results indicate that addressing chronic bacterial infection and the resulting inflammation could offer a novel treatment approach. The study also highlights the retina’s potential as a noninvasive tool for diagnosing and tracking the progression of the disease.
Read the original article on: SciTechDaily
Read more: Small Adjustment in Airflow Lowers Indoor Infection Risk by Up to 90%