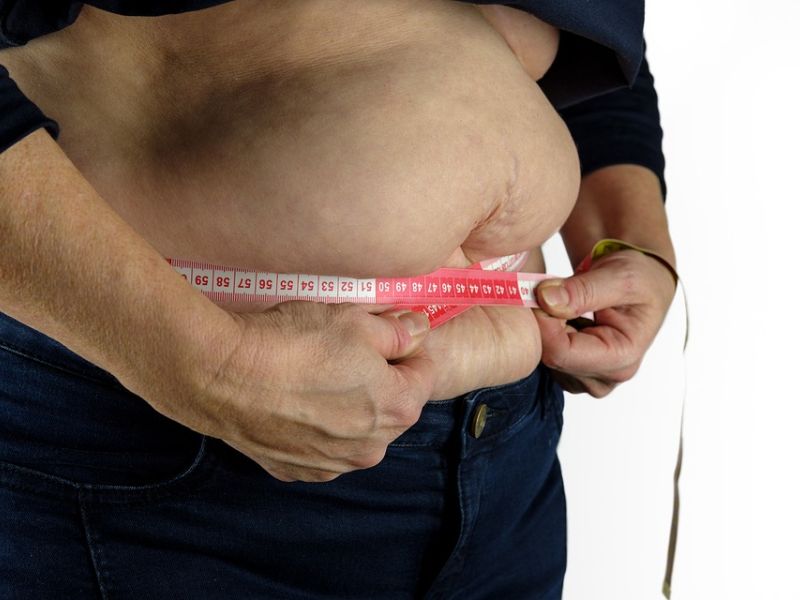
Recent studies show that chemicals in everyday plastics may silently cause long-term health issues. Early-life exposure has been associated with obesity, infertility, and cognitive impairments.
Researchers note that while minor lifestyle adjustments can help, long-term protection will demand decisive global measures.
Growing Worries Over Early-Life Plastic Exposure
Experts at NYU Langone Health warn that exposure to chemicals in common plastic products during childhood may pose serious health risks that persist into adulthood.
This finding is based on a comprehensive review of hundreds of recent studies published in The Lancet Child & Adolescent Health.
Research Connecting Plastic Chemicals to Health Issues
In their recent analysis, researchers review decades of evidence showing that additives in industrial and household plastics may increase the risk of disease and disability, particularly with early-life exposure. The review focuses on three key chemical groups: phthalates, which add flexibility; bisphenols, which provide rigidity; and perfluoroalkyl substances (PFAS), which make products heat- and water-resistant.
The studies tracked thousands of pregnant individuals, fetuses, and children, linking these chemicals to long-term health issues such as heart disease, obesity, infertility, and asthma.
“Our research highlights how plastics contribute to the early development of numerous chronic diseases that persist into adolescence and adulthood,” said study lead author and pediatrician Leonardo Trasande, MD, MPP. “To ensure children remain healthy and live longer lives, we must take strong action to reduce the use of these materials,” added Trasande, the Jim G. Hendrick, MD, Professor of Pediatrics at NYU Grossman School of Medicine.
How Common Products Emit Dangerous Chemicals
Trasande points out that these chemicals are present in many everyday products, such as food packaging, cosmetics, and paper receipts. Research shows that repeatedly using, heating, or treating plastics in certain ways can release microplastic particles and nanoparticles, which people then ingest.
Studies also suggest that chemicals in plastics can trigger excessive immune responses (inflammation) and disrupt hormones that control vital biological processes. Scientists further believe these substances may affect brain development, with numerous studies linking early exposure to lower IQ and conditions like autism and attention deficit hyperactivity disorder (ADHD).
Ways Families Can Minimize Exposure
In addition to highlighting the risks, the Lancet review offers strategies for reducing plastic use and safeguarding public health.
“There are easy and affordable measures parents can take to limit their children’s exposure to plastics,” said Trasande, director of NYU Grossman School of Medicine’s Division of Environmental Pediatrics and NYU Langone Health’s Center for the Investigation of Environmental Hazards.
He recommends swapping plastic food containers for glass or stainless steel and avoiding microwaving or dishwashing plastic items to significantly reduce exposure.
Trasande also highlights the important role of pediatricians and other healthcare providers in guiding families to make safer choices. He urges clinicians to work with schools and community organizations to educate children and teens about the potential risks of plastic exposure.
Regulatory Measures and International Initiatives
At the policy level, the authors call for stricter regulations to reduce nonessential plastic use, especially in low-income communities that already face significant health disparities.
The review coincides with the latest United Nations negotiations in Geneva on the Global Plastics Treaty, an emerging agreement aimed at limiting worldwide plastic pollution, with over 100 countries backing legally binding production caps.
Trasande emphasizes that the findings highlight the urgent need for a strong global treaty to protect both human health and the environment. He notes that while the economic influence of the plastics industry is often seen as an obstacle to new regulations, the health-related costs of plastic exposure are substantial, with his team estimating around $250 billion annually in the United States alone.
Plastics and Their Impact on Healthcare
The Global Plastics Treaty will be a central focus at NYU Langone Health’s 2025 Plastics, Human Health, and Solutions Symposium. Experts will discuss the latest microplastics research, recent policy updates, and the critical role of regulations in tackling this escalating public health issue.
While the review underscores the health risks associated with plastics, the authors emphasize that the material remains vital in many medical applications. Plastics are used in equipment like ventilators and feeding tubes for premature infants, nebulizers for children with asthma, and masks that help prevent the spread of infectious diseases. The researchers clarify that their findings do not challenge the importance of plastics in healthcare but rather highlight the need to reduce unnecessary use in everyday items.
Read the original article on: SciTechDaily
Read more: New Synthetic Biomaterial May Repair Hearts, Muscles, and Vocal Cords