
Depositphotos original extended using Firefly
Some patients don’t reach weight-loss goals after bariatric surgery, but daily liraglutide injections may help them lose more weight and reduce the need for repeat surgery.
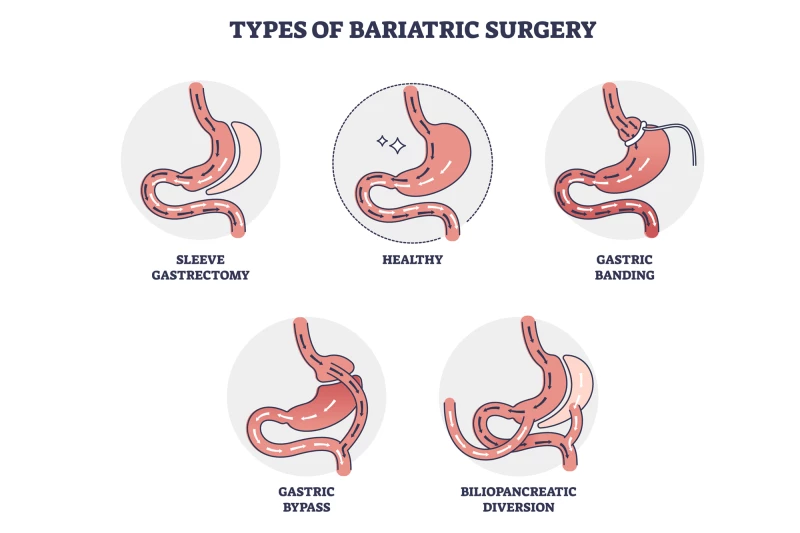
Bariatric surgery is highly effective for most with moderate-to-severe obesity, producing lasting weight loss and major health improvements, including remission of diabetes, hypertension, and sleep apnea.
Addressing Weight-Loss Plateaus with Liraglutide
However, about 15% of patients don’t lose as much weight as expected, which also limits the health benefits they gain. An Australian study now suggests that the newer injectable GLP-1 medication liraglutide may offer additional help.
“For patients regaining weight after bariatric surgery, adding medication can help, often at a lower dose,” said Professor Wendy Brown, MD, PhD.
Depositphotos
“We show patients usually don’t need the full dose of obesity medication after bariatric surgery, without affecting quality of life,” Brown said. “This could help avoid risky repeat surgery.”
The study involved 48 adults (20–65) whose weight loss 12–36 months post-bariatric surgery was below expectations. They received daily liraglutide (up to 3 mg) or placebo, with 12-month weight change as the main outcome and health markers and quality of life as secondary measures.
After 12 months, the liraglutide group lost 5.7 kg (12.6 lb) versus a 1.4 kg (3.1 lb) gain in the placebo group—a 7.1 kg (15.6 lb) difference, or 4.4% weight loss versus 1.4% gain.
Health Markers and Quality of Life
No notable differences were found between groups for blood sugar, cholesterol, or nutritional markers. Participants taking liraglutide saw a modest rise in diastolic blood pressure—from 78 to 82 mmHg. Quality-of-life scores showed small variations but no meaningful changes in overall wellbeing, mood, or eating/swallowing comfort.
Most participants didn’t reach the full 3-mg dose—averaging around 2.4 mg—but still saw meaningful weight loss. The study didn’t track why participants avoided higher doses, but researchers suggest they found it unnecessary or had mild GI symptoms. Liraglutide commonly causes nausea, vomiting, and diarrhea or constipation. The study excluded participants living over an hour away in case nausea required gastric band adjustments. Still, no serious side effects occurred, showing symptoms were generally mild and manageable.
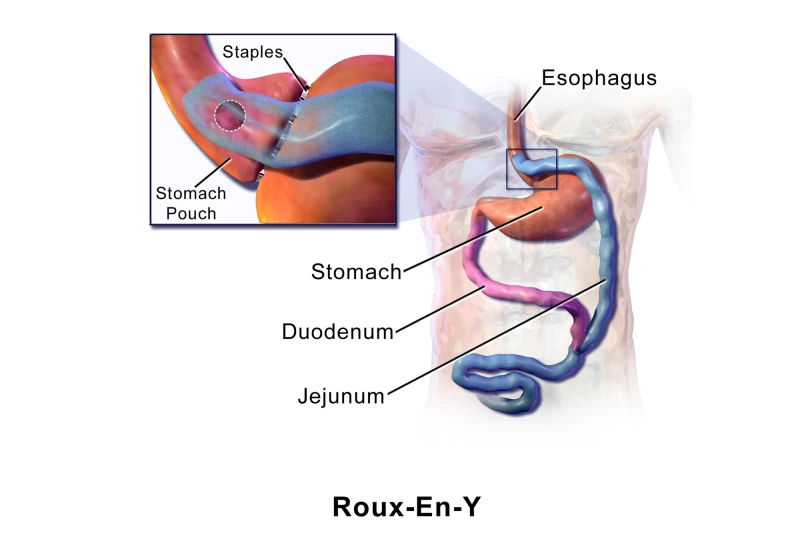
Wikimedia Commons/BruceBlaus CC BY 3.0
The researchers acknowledged several limitations in the study, including a small sample size and incomplete participation. Delays and early terminations caused by the COVID-19 pandemic and resulting drug shortages disrupted the study timeline. Most participants were women from a single center, and many didn’t reach the full liraglutide dose, leaving the impact of higher doses uncertain.
Potential of Liraglutide to Enhance Post-Surgery Outcomes
Despite limitations, liraglutide may help patients regaining weight after bariatric surgery, potentially avoiding risky repeat procedures. The study also suggests that introducing GLP-1 drugs before significant weight regain could enhance recovery outcomes. The findings suggest that combining medication with surgery could become standard for patients with partial bariatric surgery results.
“GLP-1 drugs can boost weight loss after bariatric surgery, offering hope,” said Professor John Wentworth, MD, PhD. “Even more effective, newer drugs are now available, which should help patients achieve better weight and health outcomes.”
“There are no shortcuts, but effective, evidence-based options exist,” said co-author Paul Burton, MD, PhD. “These findings support a personalized, long-term approach combining surgery, medication, and lifestyle support for lasting remission.”
Read the original article on: New Atlas
Read more: Scientists Create a Synthetic Leaf that Turns Pollution into Energy
