Samira Parhizkar/WashU Medicine
A widely available sleep aid has shown unexpected potential in supporting brain health by significantly reducing the accumulation of tau proteins — a key factor in the progression of neurodegenerative conditions such as Alzheimer’s disease.
A Cross-Continental Collaboration Aims at Innovation
This discovery stems from a collaboration between researchers at Washington University School of Medicine in St. Louis (WashU Medicine) and the Japanese pharmaceutical company Eisai. Eisai, which established a dedicated research unit in 2022 focused on Alzheimer’s prevention and treatment, is part of a growing trend that explores new therapeutic uses for existing drugs.
The team centered their research on lemborexant, a sleep aid sold under the brand name Dayvigo. Unlike traditional sedatives, lemborexant works by inhibiting orexin — a neurotransmitter involved in maintaining wakefulness — through its action as a central nervous system (CNS) depressant. Approved in late 2019 for insomnia, lemborexant belongs to a newer class of drugs called orexin receptor antagonists, which are also being studied for their potential in treating depression.
“Sleep loss has long been linked to increased risk of Alzheimer’s,” explained Dr. David M. Holtzman, senior author of the study and Professor of Neurology at WashU Medicine. “This study shows that lemborexant not only improves sleep but also reduces abnormal tau levels — a major contributor to the neural damage seen in Alzheimer’s and related disorders. We’re optimistic this could open the door to new treatments, either as standalone solutions or used in combination with other therapies.”
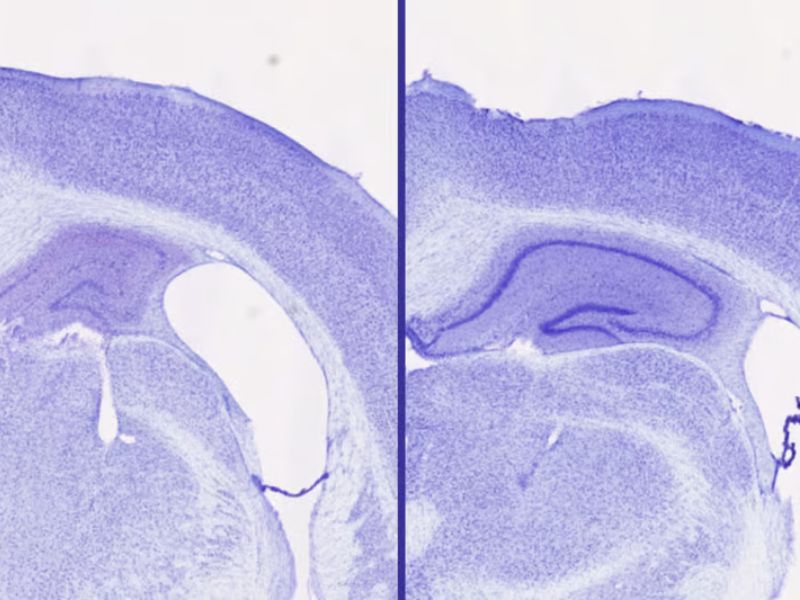
Brain Volume Preserved in Treated Mice
In the study, researchers observed genetically modified mice that were prone to developing tau buildup. They administered either lemborexant or zolpidem (brand name Ambien), a sleep aid from a different drug class that interacts with the GABA neurotransmitter rather than orexin. Despite both groups of mice sleeping similar amounts, those treated with lemborexant retained 30% to 40% more brain volume in the hippocampus — a region vital for cognitive function — than those given zolpidem. Brain volume loss is a hallmark of neurodegeneration.
Holtzman, who previously helped uncover the link between poor sleep and tau and amyloid accumulation, noted that the new findings suggest a more nuanced mechanism is at work. The ability of orexin blockers like lemborexant to reduce toxic protein deposits may offer direct neuroprotective benefits.
Interestingly, the study found these protective effects only in male mice, raising questions about biological sex differences in response to the treatment. Researchers suspect that female mice may naturally tolerate tau accumulation better, which could make the benefits of the drug harder to detect. Further investigation is needed to understand these differences.
Next Steps and Future Possibilities
Although the research is still in the animal-testing phase, the implications are promising. Orexin receptor antagonists may be particularly well-suited for use in neurodegenerative treatment regimens because they do not impair motor coordination — a concern with many traditional sleep aids.
The anti-amyloid antibody treatments we currently use for early-stage Alzheimer’s patients help, but not to the degree we’d like,” said Holtzman. “To better slow disease progression, we need strategies that also target abnormal tau and the inflammation it triggers. This type of sleep aid could become an important part of that approach.We especially want to explore whether combining therapies that target both amyloid and tau can more effectively halt or even prevent the disease’s progression.
Read the original article on: New Atlas
Read more: The US Has Recently Approved The First Blood Test For Alzheimer’s Disease