Japan is preparing to take a major step forward in medicine, as clinical trials of artificial blood that works with all blood types are set to begin this year at Nara Medical University. The research could reshape healthcare by changing how hospitals manage transfusions worldwide.
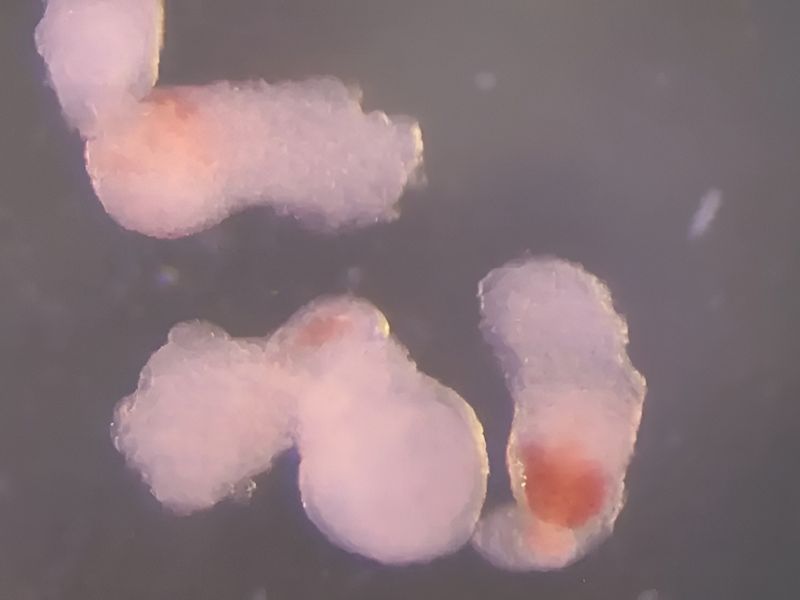
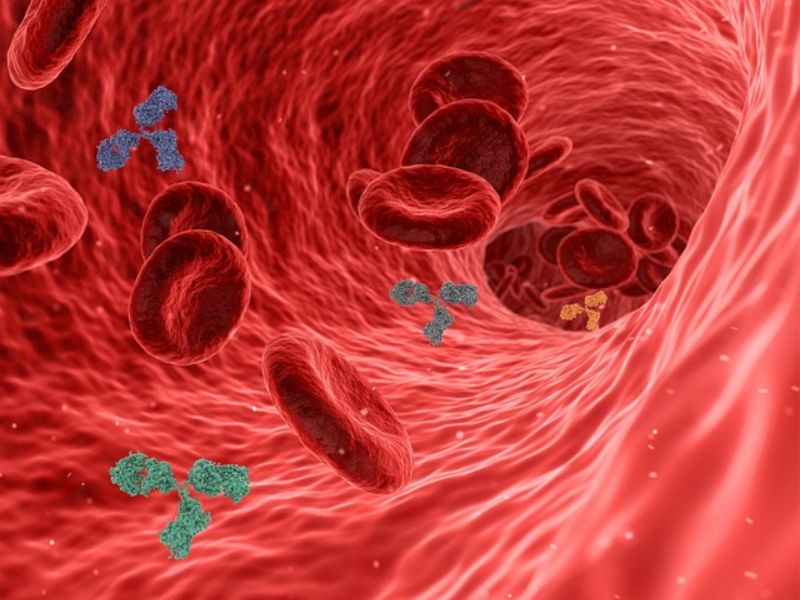
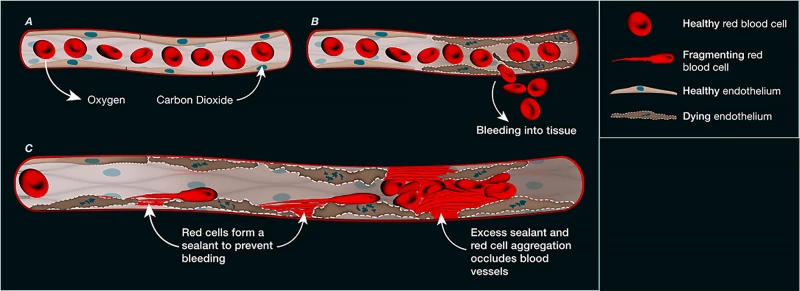
The goal is to create a universal synthetic blood that eliminates compatibility testing and expands supply. It builds on 2022 experiments with “hemoglobin vesicles,” tiny particles that carry oxygen like red blood cells. Trials in rabbits showed results comparable to real blood, without serious side effects.
Longer Shelf Life and Greater Accessibility
In addition to working for all blood types, artificial blood stores at room temperature for over a year, while donated human blood requires refrigeration and expires quickly. This could make the technology especially valuable in remote areas, disaster zones, and regions affected by conflict.
The next phase will involve human volunteers, who will receive between 100 and 400 milliliters of the artificial blood as researchers assess its safety. The long-term goal is to make the product widely available in hospitals by 2030.
This technology could help address one of the greatest challenges facing healthcare systems globally: blood shortages. Many countries struggle to maintain adequate supplies through voluntary donations alone, particularly in lower-income regions. Even in wealthier nations, patients with rare blood types often face difficulties finding compatible donors.
Addressing Blood Shortages in an Aging Society
Japan, which has an aging population and a declining birth rate, already faces growing pressure on its blood supply. Researchers are developing artificial blood from hemoglobin taken from expired donations, sealed to prevent immune reactions.
Another promising method uses hemoglobin wrapped in proteins known as albumins. Animal studies have shown that this approach can help maintain blood pressure and may prove useful in treating conditions such as severe bleeding and stroke.
According to the World Health Organization, more than 100 countries rely on imported blood products, which can limit care for patients with serious medical needs. A stable, universal synthetic blood could provide a lasting solution to this global issue.
Project leader Professor Hiromi Sakai says the advances could secure a stable, long-lasting blood supply with less reliance on donations. If successful, Japan could lead one of the century’s biggest medical breakthroughs.
Read the original article on:cff
Read more:Brain-Inspired AI Supports Stable Task Switching for Soft Robotic Arms