KOMMERS/Unsplass
Scientists have uncovered a brain circuit responsible for the emotional impact of pain, shedding light on why certain physical injuries lead to prolonged suffering. This discovery challenges existing views on pain processing and could revolutionize the way chronic pain is treated.
Pain consists of several key elements, with two primary ones being the sensory and affective components. The sensory aspect involves the physical characteristics of pain—its intensity, location, nature, and duration—while the affective component relates to the emotional experience, including the discomfort, distress, and the urge to relieve the pain.
New research from the Salk Institute has pinpointed a distinct brain circuit in mice that converts the physical feeling of pain into emotional distress.
Salk Researchers Find Sensory Pain Pathway Also Drives Emotional Suffering, Challenging Long-Held Beliefs
“For years, the dominant belief was that the brain handles the sensory and emotional aspects of pain through separate circuits,” said Dr. Sung Han, associate professor at Salk and lead author of the study. “However, there has been ongoing debate over whether the sensory pain pathway also plays a role in the emotional experience. Our findings offer compelling evidence that a branch of the sensory pathway is directly involved in generating the emotional impact of pain.”
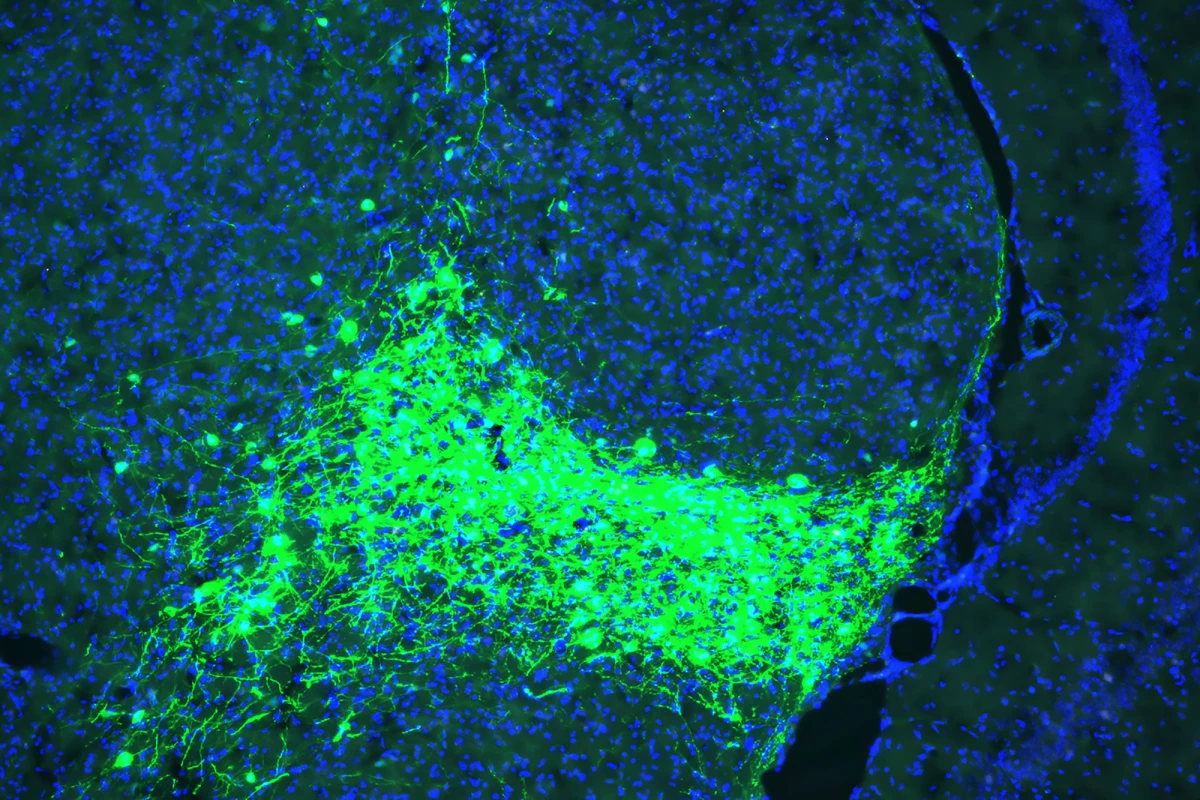
The researchers mapped the path of pain signals traveling from the spinal cord to the brain in mice. They discovered that a cluster of CGRP-expressing neurons located in the parvicellular subparafascicular thalamic nucleus (SPFp)—part of the thalamus, the brain’s central hub for sensory information—received these pain signals and relayed them to emotion-related areas of the brain, such as the amygdala. CGRP, or calcitonin gene-related peptide, is a neuropeptide that plays a key role in pain transmission.
When these CGRP neurons were genetically deactivated in mice, the animals still sensed physical pain from stimuli like heat or pressure but showed no emotional reaction and didn’t avoid the painful stimuli later. In contrast, when the neurons were artificially activated, the mice responded with fear and avoidance behaviors—even in the absence of actual pain.
Salk Institute
Study Reveals Why CGRP-Blocking Drugs Ease Pain
Drugs that block CGRP are already used to treat migraines, and this study helps explain why they’re effective—not only do they dampen pain signals, but they also reduce the emotional response that turns pain into distress. Conditions like fibromyalgia, migraines, and chronic back pain often come with emotional suffering that can be more debilitating than the physical pain itself. The research highlights CGRP neurons in the SPF as a promising target for therapies aimed at easing the emotional intensity of pain while preserving basic pain sensitivity.
“Pain processing isn’t just about nerves sensing pain—it’s also about the brain deciding how much that pain should matter,” said lead author and Salk neuroscientist Sukjae Kang. “By understanding the biology behind these two different processes, we can develop treatments for types of pain that don’t respond to standard medications.”
Because this pathway connects to emotional brain regions like the amygdala, it may also play a role in threat sensitivity and fear—key features of post-traumatic stress disorder (PTSD). Calming this circuit could help alleviate the emotional suffering tied to trauma.
The findings also open new avenues for studying how this same brain pathway might influence emotional pain from social experiences like grief, loneliness, or heartbreak.
“Our identification of the CGRP-related emotional pain circuit gives us a biological explanation for the difference between simply detecting pain and truly suffering from it,” said senior author Sung Han. “We’re eager to explore this further and work toward therapies that can help reduce emotional suffering.”
Read the original article on: New Atlas
Read more: New Brain Research Shows Dopamine Operates In a Completely Unexpected Way