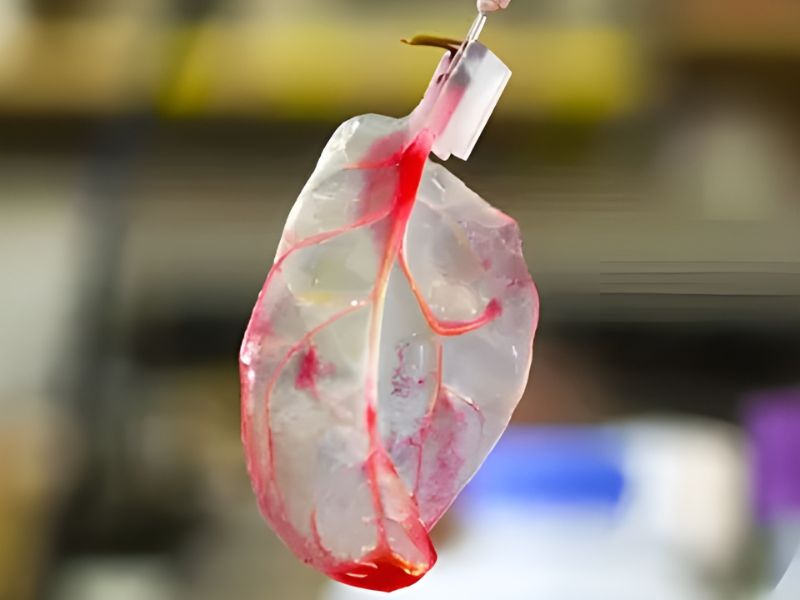
Medical progress doesn’t always come from cutting-edge technology or sophisticated machinery; sometimes it starts with simple observation. That was the case when scientists examined a spinach leaf and recognized its potential as the foundation for an experimental artificial heart, created in the lab to support research on heart disease and tissue regeneration.
The study was conducted by researchers at Worcester Polytechnic Institute in the United States and published in 2017 in the journal Biomaterials.
A Renewed Spotlight on an Unconventional Breakthrough
While the research is not new, it has regained attention in recent years for its unusual solution to one of medicine’s biggest challenges: developing living heart tissue with a working circulatory system.
Cardiovascular diseases remain the leading cause of death worldwide.
Meanwhile, the number of available organs for transplantation falls far short of patient needs.
In this context, studies focused on artificial hearts and tissue engineering have become increasingly important.
Rather than aiming to fully replace the human heart right away, the research seeks to create biological structures that can aid treatments, enable drug testing, and eventually help reduce reliance on organ transplants.
Nature’s Blueprint for Blood Circulation
These naturally branching patterns are similar to the network of human blood vessels. Because of this resemblance, researchers proposed that the leaf could serve as a natural blueprint for fluid flow, an essential feature of any artificial heart.
To allow the introduction of human cells, all of the plant’s original cells had to be removed.
This step, called decellularization, strips away the living plant tissue while leaving the leaf’s structural framework intact.
The result was a clear, lightweight, and durable cellulose scaffold that preserved the leaf’s internal channels, forming a network capable of efficiently transporting fluids.

With the scaffold prepared, the researchers seeded the spinach framework with human heart muscle cells.
From that point, the experiment entered its most carefully monitored stage.
Within days, the cells began to arrange themselves and display characteristics typical of living tissue.
Scientists observed spontaneous contractions under a microscope, signaling activity similar to that of functional heart muscle.
Testing the Leaf’s Ability to Circulate Fluids
To determine whether the plant-based structure could perform one of the heart’s most complex roles—circulation—the team injected blood-like fluids into the leaf’s veins.
The fluid moved smoothly and continuously through the spinach’s internal network.
This outcome was especially significant, as insufficient vascularization remains one of the biggest challenges in developing lab-grown tissues and artificial hearts.
Despite these promising findings, researchers stress that the model is still far from clinical use.
At present, it serves mainly as an experimental platform for research.
Even so, the method may aid in the development of tissues to treat heart attacks, cardiac injuries, and congenital defects.
In addition, scientists are experimenting with other plant species, broadening the potential applications of this strategy.
An Innovative, Low-Cost, and Sustainable Approach
Using a spinach leaf as the basis for an artificial heart stands out not only for its originality but also for its affordability and environmental sustainability.
The study highlights how innovative breakthroughs can arise from simple materials when examined through a fresh scientific lens.
Although it has no immediate medical application, the research marks a meaningful advance in regenerative medicine and suggests that future cardiac therapies may be more closely linked to nature than once thought.
Read the original article on: Clickpetroleoegas
Read more:Russian Scientists Test a Plasma Engine that could Shrink Mars Travel to 30 Days